Effect of an Early Resuscitation Protocol on In-hospital Mortality Among Adults With Sepsis and Hypotension: A Randomized Clinical Trial
- PMID: 28973227
- PMCID: PMC5710318
- DOI: 10.1001/jama.2017.10913
Effect of an Early Resuscitation Protocol on In-hospital Mortality Among Adults With Sepsis and Hypotension: A Randomized Clinical Trial
Abstract
Importance: The effect of an early resuscitation protocol on sepsis outcomes in developing countries remains unknown.
Objective: To determine whether an early resuscitation protocol with administration of intravenous fluids, vasopressors, and blood transfusion decreases mortality among Zambian adults with sepsis and hypotension compared with usual care.
Design, setting, and participants: Randomized clinical trial of 212 adults with sepsis (suspected infection plus ≥2 systemic inflammatory response syndrome criteria) and hypotension (systolic blood pressure ≤90 mm Hg or mean arterial pressure ≤65 mm Hg) presenting to the emergency department at a 1500-bed referral hospital in Zambia between October 22, 2012, and November 11, 2013. Data collection concluded December 9, 2013.
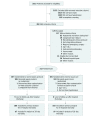
Interventions: Patients were randomized 1:1 to either (1) an early resuscitation protocol for sepsis (n = 107) that included intravenous fluid bolus administration with monitoring of jugular venous pressure, respiratory rate, and arterial oxygen saturation and treatment with vasopressors targeting mean arterial pressure (≥65 mm Hg) and blood transfusion (for patients with a hemoglobin level <7 g/dL) or (2) usual care (n = 105) in which treating clinicians determined hemodynamic management.
Main outcomes and measures: The primary outcome was in-hospital mortality and the secondary outcomes included the volume of intravenous fluid received and receipt of vasopressors.
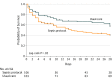
Results: Among 212 patients randomized to receive either the sepsis protocol or usual care, 3 were ineligible and the remaining 209 completed the study and were included in the analysis (mean [SD] age, 36.7 [12.4] years; 117 men [56.0%]; 187 [89.5%] positive for the human immunodeficiency virus). The primary outcome of in-hospital mortality occurred in 51 of 106 patients (48.1%) in the sepsis protocol group compared with 34 of 103 patients (33.0%) in the usual care group (between-group difference, 15.1% [95% CI, 2.0%-28.3%]; relative risk, 1.46 [95% CI, 1.04-2.05]; P = .03). In the 6 hours after presentation to the emergency department, patients in the sepsis protocol group received a median of 3.5 L (interquartile range, 2.7-4.0 L) of intravenous fluid compared with 2.0 L (interquartile range, 1.0-2.5 L) in the usual care group (mean difference, 1.2 L [95% CI, 1.0-1.5 L]; P < .001). Fifteen patients (14.2%) in the sepsis protocol group and 2 patients (1.9%) in the usual care group received vasopressors (between-group difference, 12.3% [95% CI, 5.1%-19.4%]; P < .001).
Conclusions and relevance: Among adults with sepsis and hypotension, most of whom were positive for HIV, in a resource-limited setting, a protocol for early resuscitation with administration of intravenous fluids and vasopressors increased in-hospital mortality compared with usual care. Further studies are needed to understand the effects of administration of intravenous fluid boluses and vasopressors in patients with sepsis across different low- and middle-income clinical settings and patient populations.
Trial registration: clinicaltrials.gov Identifier: NCT01663701.
Conflict of interest statement
Figures

Comment in
-
Trying to Improve Sepsis Care in Low-Resource Settings.JAMA. 2017 Oct 3;318(13):1225-1227. doi: 10.1001/jama.2017.10547. JAMA. 2017. PMID: 28973226 No abstract available.
-
The forgotten value of the clinical examination to individualize and guide fluid resuscitation in patients with sepsis.Crit Care. 2017 Dec 19;21(1):306. doi: 10.1186/s13054-017-1898-4. Crit Care. 2017. PMID: 29258571 Free PMC article. No abstract available.
-
Early Resuscitation for Adults With Sepsis in a Low-Income Country.JAMA. 2018 Feb 13;319(6):614. doi: 10.1001/jama.2017.20406. JAMA. 2018. PMID: 29450518 No abstract available.
-
Decision-making in the detection and management of patients with sepsis in resource-limited settings: the importance of clinical examination.Crit Care. 2018 Mar 1;22(1):53. doi: 10.1186/s13054-018-1971-7. Crit Care. 2018. PMID: 29490677 Free PMC article. No abstract available.
References
-
- Kaukonen K-M, Bailey M, Suzuki S, et al. Mortality related to severe sepsis and septic shock among critically ill patients in Australia and New Zealand, 2000-2012. JAMA. 2014;311(13):1308-1316. - PubMed
-
- Rivers E, Nguyen B, Havstad S, et al. Early goal-directed therapy in the treatment of severe sepsis and septic shock. N Engl J Med. 2001;345(19):1368-1377. - PubMed
-
- Levy MM, Rhodes A, Phillips GS, et al. Surviving Sepsis Campaign. Crit Care Med. 2015;43(1):3-12. - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

