The Association of Health Care System Resources With Lung Cancer Screening Implementation: A Cohort Study
- PMID: 35413280
- PMCID: PMC9529611
- DOI: 10.1016/j.chest.2022.03.050
The Association of Health Care System Resources With Lung Cancer Screening Implementation: A Cohort Study
Abstract
Background: The Veterans Health Administration issued policy for lung cancer screening resources at eight Veterans Affairs Medical Centers (VAMCs) in a demonstration project (DP) from 2013 through 2015.
Research question: Do policies that provide resources increase lung cancer screening rates?
Study design and methods: Data from eight DP VAMCs (DP group) and 20 comparable VAMCs (comparison group) were divided into before DP (January 2011-June 2013), DP (July 2013-June 2015), and after DP (July 2015-December 2018) periods. Coprimary outcomes were unique veterans screened per 1,000 eligible per month and those with 1-year (9-15 months) follow-up screening. Eligible veterans were estimated using yearly counts and the percentage of those with eligible smoking histories. Controlled interrupted time series and difference-in-differences analyses were performed.
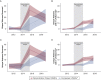
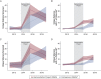
Results: Of 27,746 veterans screened, the median age was 66.5 years and most were White (77.7%), male (95.6%), and urban dwelling (67.3%). During the DP, the average rate of unique veterans screened at DP VAMCs was 17.7 per 1,000 eligible per month, compared with 0.3 at comparison VAMCs. Adjusted analyses found a higher rate increase at DP VAMCs by 0.93 screening per 1,000 eligible per month (95% CI, 0.25-1.61) during this time, with an average facility-level difference of 17.4 screenings per 1,000 eligible per month (95% CI, 12.6-22.3). Veterans with 1-year follow-up screening also increased more rapidly at DP VAMCs during the DP, by 0.39 screening per 1,000 eligible per month (95% CI, 0.18-0.60), for an average facility-level difference of 7.2 more screenings per 1,000 eligible per month (95% CI, 5.2-9.2). Gains were not maintained after the DP.
Interpretation: In this cohort, provision of resources for lung cancer screening implementation was associated with an increase in veterans screened and those with 1-year follow-up screening. Screening gains associated with the DP were not maintained.
Keywords: early detection of cancer; implementation; lung cancer screening; lung neoplasm; policy; utilization.
Published by Elsevier Inc.
Figures

References
-
- de Koning H.J., van der Aalst C.M., de Jong P.A., et al. Reduced lung-cancer mortality with volume CT screening in a randomized trial. N Engl J Med. 2020;382(6):503–513. - PubMed
-
- Moyer V.A., United States Preventive Services Task Force Screening for lung cancer: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med. 2014;160(5):330–338. - PubMed
-
- Wood DE, Kazerooni EA, et al. NCCN Clinical Practices Guidelines in Oncology (NCCN Guidelines) for lung cancer screening version 1.2021. 2021. National Comprehensive Cancer Network website. Accessed January 3, 2021. https://www.nccn.org/

