Genetic background of high blood pressure is associated with reduced mortality in premature neonates
- PMID: 31201254
- PMCID: PMC7063394
- DOI: 10.1136/archdischild-2019-317131
Genetic background of high blood pressure is associated with reduced mortality in premature neonates
Abstract
Objective: The aim of our study was to determine if a genetic background of high blood pressure is a survival factor in preterm infants.
Design: Prospective cohort study.
Setting: Patients were enrolled in 53 neonatal intensive care units.
Patients: Preterm infants with a birth weight below 1500 g.
Exposures: Genetic score blood pressure estimates were calculated based on adult data. We compared infants with high genetic blood pressure estimates (>75th percentile of the genetic score) to infants with low genetic blood pressure estimates (<25th percentile of the genetic score).
Main outcome measures: Lowest blood pressure on the first day of life and mortality.
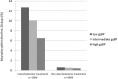
Results: 5580 preterm infants with a mean gestational age of 28.1±2.2 weeks and a mean birth weight of 1022±299 g were genotyped and analysed. Infants with low genetic blood pressure estimates had significantly lower blood pressure if compared with infants with high genetic blood pressure estimates (27.3±6.2vs 27.9±6.4, p=0.009, t-test). Other risk factors for low blood pressure included low gestational age (-1.26 mm Hg/week) and mechanical ventilation (-2.24 mm Hg, p<0.001 for both variables, linear regression analysis). Mortality was significantly reduced in infants with high genetic blood pressure estimates (28-day mortality: 21/1395, 1.5% vs 44/1395, 3.2%, p=0.005, Fisher's exact test). This survival advantage was independent of treatment with catecholamines.
Conclusions: Our study provides first evidence that a genetic background of high blood pressure may be beneficial with regard to survival of preterm infants.
Keywords: genetics; hypotension; mortality; neonatology.
© Author(s) (or their employer(s)) 2020. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: None declared.
Figures
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical